
As researchers race to find successful treatments and an eventual cure for COVID-19, everyone is getting a real-time glimpse into the messiness of scientific discovery. We’re all impatient for solid recommendations based on rigorous testing and established facts, but in a fast-moving field, that’s rarely possible. And someone always has to be the guinea pig. This was just as true 130 years ago when Niels Ryberg Finsen began experimenting with treating disease with UV light. He started by testing on himself.
The germ-killing properties of the sun
Finsen was far from the first to consider the disease-fighting effects of light. By the end of the 19th century, the germ theory of disease had taken root, and doctors and scientists eagerly sought treatments that had antimicrobial properties. One of the earliest sources of hope was simple sunlight.
In the 12 July 1877 issue of Nature, public health experts Arthur Downes and Thomas P. Blunt published a short note called “The Influence of Light Upon the Development of Bacteria” [subscription required]. Their claim: Sunlight is inimical to bacteria. The authors recognized that it had long been known that light was not essential for the development of germs, but they thought they were the first to systematically study the effects and prove that sunlight destroyed bacteria.
Downes and Blunt were clear in their stated intentions: They wanted to link observed facts to the underlying chemical processes, and then to extend their observations to other phenomena. They were also clear on the limits of their inquiry. Although they hoped to report on the influence of refracted sunlight, they reached no definitive conclusions.
Their report touched off a flurry of scientific inquiry. John Tyndall, a physicist and Fellow of the Royal Society, attempted to reproduce Downes and Blunt’s experiments, albeit under slightly different circumstances. Downes and Blunt had used thin glass test tubes containing a sterilized Pasteur salt solution, which they monitored under direct and indirect sunlight in suburban London. Tyndall conducted his experiments in the Alps with hermetically sealed flasks of infusions of cucumber and turnip.
Tyndall’s initial findings aligned with those of Downes and Blunt: Flasks exposed to strong sunlight remained free of bacteria. But when Tyndall moved them to a warm room, they developed bacteria. This led him to conclude that sunlight only suppressed the growth of bacteria rather than killing it outright.
Tyndall published his results in the 19 December 1878 issue of the Proceedings of the Royal Society of London, ending his report almost apologetically: “I do not wish to offer these results as antagonistic to those so clearly described by Dr. Arthur Downes and Mr. Thomas Blunt.... Their observations are so definite that it is hardly possible to doubt their accuracy. But they noticed anomalies which it is desirable to clear up.... Such irregularities, coupled with the results above recorded, will, I trust, induce them to repeat their experiments, with the view of determining the true limits of the important action which those experiments reveal.”
It was a polite but firm takedown. More work was needed to elucidate the science behind the germ-killing effects of sunlight.
Over the next two decades, the messiness that is the process of discovery continued to play out as investigators nailed down details in different experiments. Downes and Blunt went on to demonstrate that the effectiveness of light to neutralize bacteria depended on the light’s intensity, duration, and wavelength. Later researchers repeating Tyndall’s experiments determined that the high particle concentration in his flasks shielded some of the bacteria from the sun’s damaging rays. Numerous scientists questioned, confirmed, extended, and complicated these initial claims, as Philip Hockberger, a physiologist at Northwestern University, has outlined in his review of the history of ultraviolet photobiology.
The Finsen lamp treated tuberculosis of the skin
Niels Ryberg Finsen entered into this fray in the 1890s. Despite an unimpressive school record, he had studied medicine at the University of Copenhagen. Following his graduation in 1890, he got a job preparing dissections for anatomy classes, but he quit after three years to focus on his research.
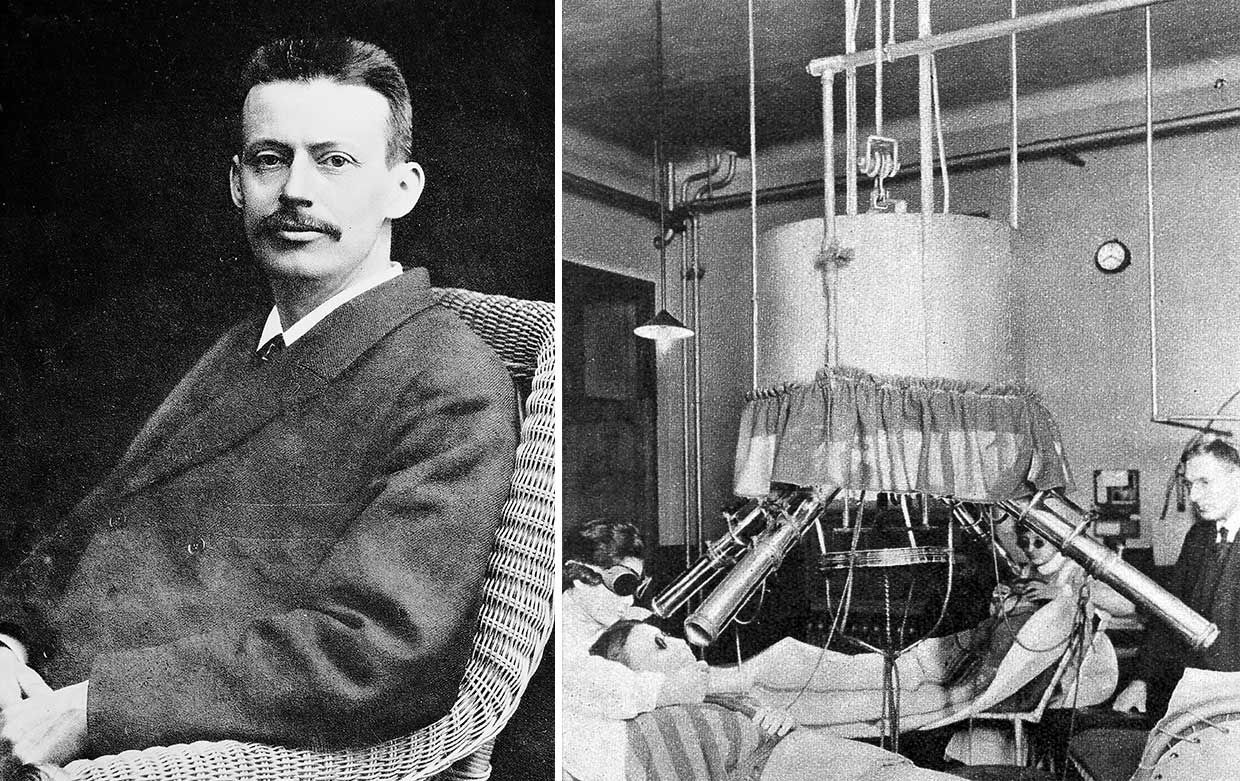
Niels Ryberg Finsen showed that UV light could cure tuberculosis of the skin. His lamp could treat multiple patients at the same time.
Finsen’s personal experience with illness prompted his investigations into the medicinal qualities of light. While in his 20s, he developed what is now known as Niemann-Pick disease, a rare genetic disorder that affects the body’s ability to metabolize fats. His initial symptoms included anemia and fatigue; by the time he died at age 44, he was in a wheelchair. Because Finsen lived in a north-facing house, he wondered if more exposure to sunlight would help. But being a medical man, he also thought it would be inappropriate to apply a theory if it were not built upon scientific fact. He decided to undertake formal studies of both sunlight and artificial light.
Finsen began with the effects of sunlight on insects and amphibians, publishing papers in 1893 and 1894, but he soon turned to the effectiveness of artificial ultraviolet light. Light rays outside of the visible spectrum and adjacent to the blue-violet were then known as “chemical rays,” because of their ability to stimulate chemical reactions, such as oxidizing the metallic salts used in early photography. Chemical rays were distinct from the “heat rays” adjacent to the red-orange end of the visible spectrum and now known as the infrared.
There were many conditions that Finsen thought might benefit from UV light, including smallpox, typhoid, and anthrax. But he had to start somewhere, and he made his choice almost at random. In 1895 he had arranged to use the laboratory of the Copenhagen Electric Light Works. One of their engineers, Niels Mogensen, suffered from lupus vulgaris, a skin condition that results in disfiguring lesions on the neck and face, caused by the same bacterium responsible for tuberculosis in the lungs. Having already tried medication and surgery, Mogensen was willing to be Finsen’s guinea pig. After only four days of treatment with artificial light, he showed improvement.
Finsen published the first report of his findings the next year, with details on 11 patients with lupus vulgaris. Critics claimed that the sample size was too small, but Finsen responded that because the treatment was localized—light directed at a specific spot for a fixed duration—the causality was clear. Score one for clinical tests.
For his treatments, Finsen developed an electric carbon arc light that became known as the Finsen lamp. Initially, he used regular glass in the lens, but soon replaced it with a fused quartz lens that provided more uniform transmission of UV rays. A single lamp could have four to eight tubes or arms, each of which looked like a telescope. The tubes could direct light to multiple patients at the same time.
A nurse would press a disk firmly against the patient’s skin to prevent blood from entering the treatment area and hindering the light’s penetration. The light was so intense that both patients and medical practitioners wore dark glasses to shield their eyes. Treatment occurred daily, lasting for 1 to 2 hours per day. Mild cases could be cured in a matter of weeks, but the average treatment lasted about seven months, with severe cases taking over a year.
With the help of the mayor of Copenhagen and some philanthropic donors, Finsen established the Medical Light Institute to treat lupus vulgaris. On 12 August 1896, the institute welcomed its first two patients. By 1901 it had treated 804 patients and claimed an impressive cure rate of 83 percent. Patients came from across Denmark and Europe, paying the equivalent of US $18 per month for Danish citizens and $30 for foreigners. Danes without the means to pay had their costs defrayed by their home districts.
As word of Finsen’s success spread, Finsen Institutes began popping up across Europe and North America. In 1900, Princess Alexandra, wife of the future King Edward VII of the United Kingdom, was instrumental in bringing the Finsen lamp to the U.K. Alexandra was Danish and supported the work of her countrymen. She presented a lamp to the Royal London Hospital, one of the lenses of which is featured at top.
Other forms of light therapy, based on sunlight and artificial light, also grew in popularity, for treating TB, circulatory disorders, varicose veins, degenerative diseases, and delicate constitutions. Light therapy for pets was faddish for a time, too.

As might be expected, some of the treatments for both humans and animals didn’t hold up to scientific scrutiny. In 1928, for example, the medical researcher Dora Colebrook published in The Lancet a study of 237 children that showed no beneficial effects of therapy with sunlight or artificial light. She was swiftly denounced in both medical journals and popular newspapers. The public—and many practicing physicians—were convinced it worked, and treating patients and building the associated electrical equipment were big business.
The shift to using UV lights to disinfect
In 1903, Finsen was awarded the Nobel Prize in Medicine, although the award was not without controversy. Some critics argued that his contribution did not have sufficient theoretical backing, which Finsen didn’t deny. But he contended that if clinical experiments alone could lead to the treatment of disease, it served no purpose to wait until an explanation was found in a lab. Other critics saw his investigations as superfluous, considering that knowledge of the bactericidal effects of UV light had been known for decades.
Meanwhile, supporters found his treatment innovative and in the spirit of Alfred Nobel because it benefited humanity. Those who suffered from lupus vulgaris faced discrimination and ostracism. In fact, Finsen’s out-of-town patients sometimes had trouble obtaining lodging due to their appearance. That predicament was remedied when two former patients established a boarding house for those undergoing treatment, which turned out to be a very lucrative investment. Finsen’s phototherapy transformed his patients’ appearances and allowed them to live normal, active, social lives.
Finsen was too sick to attend the Nobel Prize ceremony, and he died less than a year later. He donated a significant portion of his prize money to his institute, which was matched by two other donors. He also gave a large sum to a sanatorium for heart and liver disease.
The use of phototherapy for lupus vulgaris eventually declined, especially after penicillin became widely available. The Royal London Hospital’s lamp was repurposed to treat rickets. In 1953, the hospital transferred the lamp to the Wellcome Institute for the History of Medicine, and it now resides in the collections of the Science Museum, London.
But even as Finsen lamps were being retired, research on UV light was taking off in a new direction: killing germs in the environment before they had a chance to infect anyone.
In the 1930s, William F. Wells, an instructor in sanitary science at the Harvard School of Public Health, introduced the idea of aerosolized infection—droplets containing an infectious disease suspended in the air for hours. He postulated that a room could be rid of these airborne germs by an ultraviolet lamp and proper air circulation.
UV ventilation systems were soon being installed in schools and barracks with the hope of controlling the spread of tuberculosis and measles. Several later studies, though, were unable to reproduce Wells’s success. But Richard Riley, a medical student who worked in Wells’s lab, continued to believe and to research the effects of UV ventilation systems.
During the early 1970s, Riley and his colleagues published numerous papers that confirmed aerosolized TB could be controlled through UV ventilation. They also showed that relative humidity, temperature, the placement of the lights, and airflow affected how well it worked. In the 1980s, the United States saw a spike in tuberculosis, some strains of which were resistant to antibiotics, and interest in Riley’s and Well’s research was renewed.
UV lights were also found to disinfect drinking water and kill germs on surfaces. The first UV water treatment plant was prototyped in Marseilles, France, in 1910, but the lamp technology needed to improve before the technology could see widespread adoption. Commercial water treatment with UV began in the 1950s and really took off after research in 1998 showed that UV was effective at killing chlorine-resistant protozoa, such as giardia and cryptosporidium. Today, there are a whole host of consumer products that tout the benefits of UV sterilization. I recently bought my mom one of those pouches that have tiny UV lights for sterilizing your keys and cellphone.

These days, the germicidal benefits of both sunlight and artificial UV light are back in the spotlight as potential weapons against the coronavirus. Much is still unknown about the virus that causes COVID-19—how it spreads, whether immunity is short-lived or enduring, why the list of symptoms keeps growing, why it makes some people very sick and others not at all. As we watch this scientific process play out in real-time, it might be helpful to remember the words of Finsen upon his acceptance of the Nobel Prize: “The supreme qualities of all science are honesty, reliability, and sober, healthy criticism.” Trial and error, proposal and critique, success and failure are all part of the messiness of science.
An abridged version of this article appears in the September 2020 print issue as “The Healing Light.”
Part of a continuing series looking at photographs of historical artifacts that embrace the boundless potential of technology.

